Updated: April 7th, 2023
Published: March 17th, 2023
Updated: April 7th, 2023
Published: March 17th, 2023
Organizations typically either require all providers to have some type of basic or advanced life support or they require some specialties to maintain certification. This paper has been written to provide education to Medical Services Professionals about the providers of basic and advanced life support, how criteria should be written and other issues that are relevant and important for an organization to consider when establishing their internal standards.
The Use of Criteria in Privileging
During the early years of privileging (1970s and early to mid-1980s), privileging criteria was scarce – almost non-existent. Privileges were laundry lists and there wasn’t a lot of emphasis on confirmation of current clinical competency prior to granting privileges. Typical criteria included items that we would consider today to be more related to membership criteria – such as living within a certain distance from the hospital, having malpractice insurance, etc. When privileging criteria began to be incorporated into privileging decisions by healthcare organizations, it was typically because something new had been introduced – some type of device or new methods of performing procedures.
Privileging criteria became much more widely used beginning in the early 1990s due to the impact of the National Practitioner Data Bank when it became understood that an organization didn’t have to deny a provider a privilege if the provider didn’t meet the stated threshold eligibility requirements for the privilege. This was advantageous to both the provider (because he/she wouldn’t have a denial of privileges on his/her record and a report to the NPDB) and for the organization (because there is no report to the NPDB, there is no requirement for a hearing).
As criteria became more widely implemented, it also moved from separate policies and procedures to being defined on the privilege delineation itself. The reason for this, of course, is that organizations want the criteria to be clearly visible to applicants for privileges as well as to those who recommend privileges.
Today, criteria is fundamental to the privileging process because the Centers for Medicare and Medicaid Services (CMS) are extremely direct in their requirements that privileging be criteria-based (and CMS requirements drive the standards of the accrediting organizations, such as The Joint Commission, that have “deemed status” with CMS).
The following is an excerpt from a November 12, 2004 letter (the complete document is attached to this document) from the CMS directed to State Survey Agency Directors related to how privileging must be surveyed.
The hospital must have a privileging process in place that complies with CMS requirements. The hospital’s privileging process must be in compliance with the hospital CoPs at §482.12 (Governing Body), §482.22 (Medical Staff), and with other CoPs that require medical staff oversight of practitioner qualifications and privileges, federal and state law, and the process must be approved by the hospital’s Governing Body. The hospital’s Medical Staff bylaws must describe the privileging process to be used in the hospital. The process must include criteria for determining the privileges that may be granted to individual practitioners and a procedure for applying the criteria to individual practitioners.
We recommend that privileging criteria be clear and concise – and most importantly, be consistently applied. And we must always remember that the goal of privileging is to assure that only providers who can demonstrate competency are granted clinical privileges – thus providing benefit and protection to patients.
As we explore requirements related to certification for basic and advanced life support, we must remember that certification is criteria that relates to the exercise of specific privileges. It is not a privilege by itself or that stands alone. Below is an example of “what not to privilege”.
Don't Do This
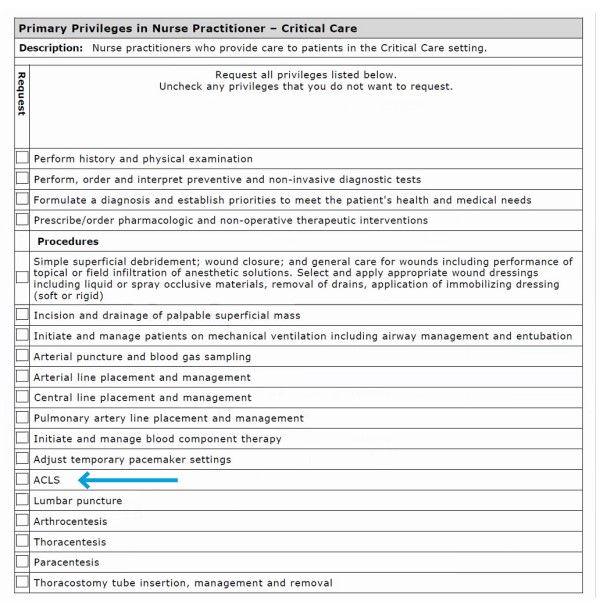

Certifications for Basic, Advanced Life Support and Pediatric Advanced Life Support (BLS, ALS and PALS)
Looking Back at Requirements for Life Support Certification
Many medical staff organizations in the past required basic or advanced life support as a requirement of medical staff membership or as a requirement for any type of clinical privileges. The reason for requiring certification was to assure a basic level of competency for all providers (including nursing) to identify and reverse a cardiac or respiratory arrest (basic life support) or to support the patient (advanced life support). In the 1980’s, when many hospitals implemented Code Teams, it was important to identify what providers could lead the team as well as those who could serve as a team member. And – at that time, because of the variations in training in residency programs, it could not be assumed that the skills to lead a team were always incorporated into residency training programs. Therefore, certification in basic and/or advanced life support was a credential that became vital to many healthcare providers and hospitals.
If basic or advanced life support was a membership requirement, it was included in the medical staff bylaws and listed with other membership requirements. If it was a basic requirement for clinical privileges, it was included in the bylaws article related to clinical privileges. Or sometimes the requirement was listed in the medical staff rules and regulations. In many cases, the requirement was written as “basic” or “advanced life support certification” from the American Heart Association (AHA). And, as often occurs with these types of documents, they do not get changed until it becomes apparent that an update needs to be made, as is occurring today because of another option for training and certification – the American Red Cross (ARC).
Facts Related to BLS, ALS and PALS
- The International Liaison Committee on Resuscitation (ILCOR) is the organization that sets international guidelines for resuscitation. ILCOR’s evidence evaluation is undertaken and lead by ILCOR’s member organizations and other evidence based national and international leaders in resuscitation such as the American Red Cross and the International Federation of Red Cross and Red Crescent Scotties (IFRC). These guidelines are referred to as CoSTR (Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations). ILCOR was formed in 1992 as a not-for-profit organization to develop and disseminate international consensus statements or guidelines for resuscitation. National organizations who provide evidence based training such as the American Red Cross and the American Heart Association take the ILCOR CoSTR and adapt them as appropriate to their regions. For example, some 23% of deliveries in The Netherlands occur at home, and The European Resuscitation Council standards reflect this divergence from the international norm. In the past while both the ARC and AHA took the ILCOR guidelines and adapted them to the US, the AHA was the only organization to offer ALS and PALS. That is why when discussing ALS and PALS, many refer to the guidelines as being from the AHA when in fact the origin of guidelines is ILCOR, which are then the basis for both the ARC and AHA programs.
- Training and certification from the American Red Cross and the American Heart Association are based on the same evidence reviewed and treatment recommendations developed through the ILCOR process. Both offer classroom training with a certified instructor or online blended with a feedback manikin.
Recommendations Related to Credentialing and Privileging
1. Do not specify a specific provider of training/certification in bylaws, policies and privileging criteria.
Organizations have, in their quest to be specific, identified one provider in their documents, for example: “Current certification in ACLS from the AHA.” This therefore eliminates the possibility for healthcare professionals to seek certification from educational providers who offer equivalent and in the view of some students and organizations preferred programs such as that offered by the American Red Cross. See #4 (below) for the way that criteria should be written.
2. Determine what healthcare providers must maintain certification.
It is up to each organization to determine the extent to which certification must
be maintained by healthcare providers. Some organizations want all healthcare
professionals (nursing and physicians) to maintain life support certification –
others will make their requirements specific related to the privileges held by
providers/
Medical staff bylaws, rules and regulations or policies should state either that BLS, ALS or PALS certification is required for all privileged providers (based upon their patient care responsibilities) OR that requirements related to certification for basic, advanced life support or pediatric advanced life support will be specified within applicable privilege delineations.
Appropriate Method of Documenting Criteria on a Privilege Delineation (s for a Nurse Practitioner-Critical Care)
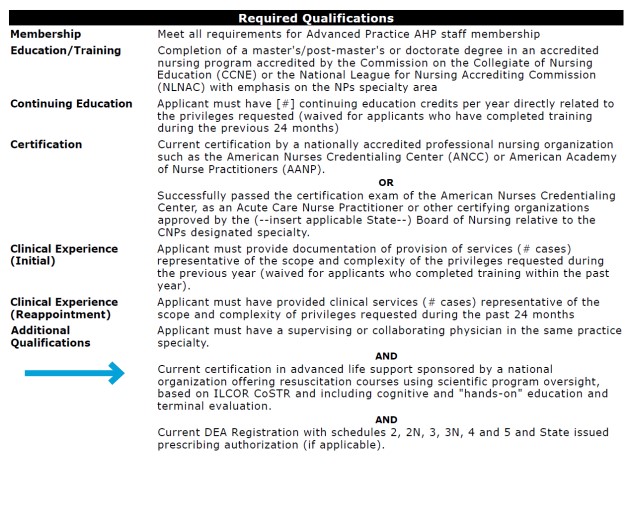
3. Specify the type of training
that qualifies.
Providers of training/
certification must provide
training and certification
based on ILCOR guidelines.
Additionally, skills validation is
required to be a component
of the curriculum (i.e., the
certification cannot be
based on training exclusively
obtained online).

4. If life support requirements are related to specialties, determine the privileging criteria and the specialties to which the criteria is applicable.
Privileging criteria should be written to be unambiguous. Here is an example: “Current certification in (insert type of certification that is required - i.e., ALS, PALS) sponsored by a national organization offering resuscitation courses using scientific program oversight, based on ILCOR CoSTR and including cognitive and “hands-on” education and terminal evaluation.”
5. Determine timeframes for validation of certification.
Consider pros and cons when options for verification timeframes are selected. The options include:
Initial credentialing: Verification of current certification as required. k At expiration or renewal of privileges: ( At expiration of the credential ( Verify currency at renewal of applicable privileges (i.e., every two years)Determination of the appropriate option should consider the following: Is it more important to target your management systems to enforcing expiration? Or is it more important that the privilege holder review and update their skills and recertify every two years? If the applicable certification is updated at the time of recredentialing, there is plenty of advance notice of the pending renewal of privileges and the requirements that must be met at that time – and it is less likely that there will be lapses in privileging due to expiration of life support certification.
If your organization determines that it is appropriate to update every two years (rather than at expiration) your privileging criteria might state: “Current certification in (insert type of certification that is required - i.e., ALS, PALS) sponsored by a national organization offering resuscitation courses using scientific program oversight, based on ILCOR CoSTR and including cognitive and “hands-on” education and terminal evaluation. Evidence of current certification is required at initial appointment and at the time of reappointment.”
6. Other considerations.
Organizations may want to provide their providers with an incentive to use a specific training and certifying organization in order to facilitate compliance with their internal requirements and to make it convenient for their healthcare providers to achieve certification. Selection of a provider of education and certification with the capacity to provide classes/programs that are readily available is essential.
At VerityStream we are proud to offer our employees and organizations training provided via the American Red Cross. The American Red Cross program is the most innovative resuscitation program in the world, leveraging the latest technologies for manikin, simulation, virtual reality, adaptive learning and more.
The ARC uses an adaptive learning model that saves individuals and organizations
significant time. Healthcare providers that can demonstrate competence up-front,
do not have to go through all of the course materials. For on-the-go learners, the
content works with smartphones, tablets, and laptops.
If your organization has a direct link into your provider/credentialing software that provides dynamic verification of basic or advanced life support from the certifying organization – your job of tracking this information is made exponentially easier! The Red Cross and Healthstream partnership allows this type of dynamic primary source verification. It also provides you a validated credential in Basic Life Support, Advanced Life Support and Pediatric Advanced Life Support.
Finally – let’s remember why life support certification is important:
When every member of the resuscitation team is both competent and confident, lives are saved.
